It’s a sad fact of life in much of the North: if you’re seriously sick, you have to leave home.
If you live in one of the territory’s larger centres, you’re lucky. Sure, you might have to fly south for some major surgery or to see a specialist. But if you break a bone or need a root canal, you can at least be assured that, at the end of the day, you’ll be resting up in bed at home.
If you live in a smaller community without all-weather road access though, you might only see a doctor or dentist or optometrist when they come through your town. Without that consistent presence, health issues that are easily preventable can develop into long-term problems that leave you in pain and lacking peace of mind. And then you have to hop on a plane, leaving friends and family, to spend days in a hospital bed or boarding home until you’re well enough to travel back.
It’s far from ideal. But those tasked with providing health care—the doctors, nurses, dentists—do what they can to ensure the 110,000 people North of 60, spread across 40 percent of the country’s landmass, can at least see someone when they really need to.

Caring for a quarter of Canada
A day in the Yellowknife Emergency Room
It’s midway through the morning when Jennifer Butler asks an elderly man if he wants her to let him die.
The emergency department physician speaks loud and slowly. She asks the man if he wants staff to “pound on his chest” if his heart stops. But the man doesn’t speak English. The information is relayed through his friend who plays translator, sitting next to his bed in the Stanton Territorial Hospital emergency room.
“There’s really no other option,” Butler says afterwards. With 11 official languages in the NWT, as well as those spoken by the growing number of tourists visiting the capital from around the globe, this isn’t her first fight to be understood. “If it’s something very complicated medically then we can get translators, but even translators realistically don’t necessarily have a whole lot of medical expertise,” she says. (Oh, and yes, the man would like to be resuscitated.)
Welcome to emergency medicine at the biggest hospital in the Northwest Territories. “We used to have this saying down here that we’re providing care for 25 percent of Canada, 24/7,” says David Pontin, lead of territorial emergency and hospital services. He gestures to a map on the wall, showing the huge swath the hospital covers, stretching throughout the NWT and into Nunavut’s Kitikmeot region.
It’s a quiet Friday morning. Butler checks to make sure a teenager has EpiPens, while a nurse finishes a snack of melted cheese on saltines before checking on a man who is vomiting. Patients wait around 30 minutes to be seen. But days earlier, it was so busy some patients waited seven hours to see a doctor. Staff had to call a surge. They do this when all 10 beds in the department are full and no more beds are available upstairs. Essentially, it’s all hands on deck. They set up chairs for patients in a hallway and call in off-shift doctors. The surge lasted nine hours—it was the fortieth such call in the last eleven months.
“Burnout is a serious epidemic within health care."
It’s been a rough year for the flu, but Pontin says that’s not the only reason they’re busier. He can’t put his finger on one clear culprit, it’s a combination of factors—from an increase in teen psychiatric cases that Pontin says have gone “off the rails” in the last three years, to a clinic shortage in Yellowknife. For people without a family doctor, the emergency room is often their only option.
Patients come in from across the territory too because they’re unable to access the care they need in their own small communities. “In some senses, it feels like you’re doing a mission to an underserviced country,” says Butler. “You have people who really just need your care. It’s not a question of, ‘Oh, which hospital will I choose?’ It’s, ‘I have to take a three-hour plane ride south to come to Yellowknife to get cared for.’”
And then there’s the high number of drug- and alcohol-related cases that fill the beds. “Frankly, the population we deal with on a routine basis here is more like an inner-city population, like we might see in downtown Vancouver, as far as the intensity of the addictions,” says Pontin. “The reality is that emergency medicine is dealing with intoxicated patients. And it’s dealing with potentially violent patients.” This contributes to burnout among staff. He says nurses last three to five years in Yellowknife, while doctors generally stick around slightly longer. “Burnout is a serious epidemic within health care,” Pontin says. He’s been at Stanton since 2006, Butler since 2010.
What keeps Pontin going is working with his team to tackle impossible situations—whether that’s entire families going through the ice in their cars or multiple plane crash survivors arriving in the emergency room. “By the end of the shift you’ve done these really great things.”
– Jessica Davey-Quantick
Growing old in the bush
A senior’s dilemma in Marsh Lake, Yukon
Annie Parker needs to get firewood in the house. She builds up her resolve, takes one last puff on the oxygen, then shuffles out the door in her big snow boots and parka. It’s -30C. The 74-year-old grapples a piece of wood out of the neat stack in her yard and scuffs back to the house, taking slow, small steps and breathing hard. Wet clacking comes with each exhale. Wispy ghosts of vapour trail out of her mouth.
She carries one log at a time, depositing them in an accumulating pile outside her backdoor. She’ll go inside and take another few draws off the oxygen tank before heading outside for more. “You have got to be determined,” says Parker. “If you’re a wussy, you shouldn’t be out in this area anyhow.”
Parker lives alone in a cozy brown cottage on a sloping, forested property overlooking Marsh Lake, an hour south of Whitehorse. She’s been widowed for six years, lives off a meagre pension, recently survived a bout of cancer but ends up doing mostly everything herself. It’s a dilemma Northerners face when they get on in age: do you stay or do you go? With few services, scant help and low incomes, an aging and ailing body challenges their steel will to stay at home. But what’s the alternative? Moving south to a more comfortable climate or into a seniors’ facility, often away from your hometown.
“I would like to stay here until I die,” Parker says. “I do what I have to do.” (Annie Parker is not her real name—she asked that Up Here not use it because she didn’t want people to think she was vulnerable. Or a whiner.)
In fact, she is wiry and strong. Three years ago, Parker was up on her roof in the dead of winter heaving and swinging the blunt end of an axe to chip away the built-up ice. “I was just a mass of bruises,” she recalls. “But I did it. Nobody else was going to do it.”
Since contracting lung cancer around five years ago, Parker has suffered from recurrent pneumonia. Last year, she got it seven times, including a bout in November that landed her in the hospital for 10 days after both lungs filled with fluid. She’s still recovering from that episode. She’s on regular oxygen. She has an air converter by her chair she calls “her great big Jesus thing,” plus backup tanks in case the power goes out. She also gets scheduled immunotherapy injections straight into a tube that runs under her skin from her elbow to her chest. It’s necessary after her veins collapsed from cancer treatments. Yukon Home Care nurses visit regularly for various treatments and check-ups. Two are coming out tomorrow but her front pathway is knee-deep in fresh snow. So out she goes.
“I would like to stay here until I die”
“I had to shovel to the gate and it’s only a shovel wide, but I really do need somebody who can do these things for me,” admits Parker. She can only afford a few services: monthly housecleaning, snow clearing for her driveway, plus firewood delivery and splitting. The rest is up to her.
Parker’s not alone. The number of rural seniors struggling to live at home is growing, as are demands for basic services—shovelling, cutting firewood, yard maintenance—that would help prevent seniors from moving into one of the Yukon’s full-to-capacity hospitals or long-term care facilities. Groups like Senior Action Yukon are pushing the government to introduce programs that would let people like Parker stay in their homes as long as they possibly can, which would be a win-win for seniors and the health care system.
“I’m by myself,” she says. “I’m not incapacitated. I can still drive my car. I just can’t do anything that requires a lot of energy. It’s the day-to-day help is what I need. If there was just somebody around here you can count on.”
– Katharine Sandiford
Robot teeth wars
A fight to prevent tooth decay in Nunavut
It has become a rite of passage for kids in Nunavut communities. A charter flies them south to places like Churchill, Manitoba, Ottawa or Edmonton. There, they sit through root canal procedures and have their tiny teeth capped with stainless steel crowns. The kids call it getting your “robot teeth.”
This doesn’t make Steven Partyka smile. The Iqaluit dentist behind Arctic Circle Dental Services calls the robot teeth “metal atrocities.”
“I don’t think it’s a very nice thing to have little children with a mouth full of metal. I think it affects their self-esteem, and kids have it tough enough these days,” he says. “I’d love to catch it way sooner—prevention is definitely the key.”
Report after report shows Nunavummiut have far higher rates of tooth decay than the national average. To combat this, Health Canada spent more than $200 million per year between 2011 and 2016 to attempt to improve oral health in First Nations and Inuit communities. Still, most Nunavut communities don’t have a full-time dentist and only get dental care when one tours through. That often means dental issues are only dealt with once they become problematic or painful. These issues could be prevented with ongoing check-ups and education.
Ron Kelly is the territorial government’s dental officer. He says the list of kids requiring major dental treatment is pushing 700. (They can help roughly 500 per year.) And the longer the wait, the worse problems get.
Kelly’s just arrived in the small community of Resolute on Cornwallis Island, where he’ll see about a dozen kids a day. Then he’ll head north to Grise Fiord for a week before looping back to see more patients in Resolute. Robot teeth aren’t ideal, he admits, but they’re better than infected teeth. “It’s going to take a while before that ship gets turned around.”
But Partyka thinks part of the problem is having fly-in dentists at all. “I would love to see some more dentistry in the communities, even if it was just longer-term positions. Consistency of care is the most important thing. How can you really treat a patient properly if you’re really not aware of their socio-economic status and their real needs? You only get to know that if you know your patients,” he says.
“I don’t think it’s a very nice thing to have little children with a mouth full of metal."
Dentists can spot symptoms of abuse, malnutrition and other issues before they’re reported, he says. “Years ago, when I first got here, we had a child just show up here because they knew it was a safe place. They had an abusive situation at home, and they just came here because they knew it was a happy place. And you just go, ‘Wow, that’s something you don’t get in downtown Toronto.’”
Kelly says many of the dentists who tour communities—like other doctors and specialists—come back year after year. He’s not sure installing dentists full-time is realistic. Take Resolute and its 250 residents. “There’s no way a full-time dentist would come here. They’d starve to death.”
– Jessica Davey-Quantick
Real good midwives of Nunavik
A comfortable childbirth in Puvirnituq
Tom Unaluk is a curious and active 18-month-old. He’s starting to say a few words in Inuktitut. He learns fast, says his mother Leah from her home in Puvirnituq, Nunavik, in Northern Québec.
Tom was born August 19, 2016 at the Puvirnituq Maternity Centre. It’s less than five minutes from their house by car. That’s good news since Leah’s partner had to rush her there when her water broke shortly after 2 a.m. They didn’t even have time to call family and friends, but they passed on the happy news in the morning. Leah and Tom went home the next day.
Along the eastern coast of Hudson Bay, 86 percent of births are attended by midwives—many of them Inuit. There’s a focus on traditional birthing practices from before the 1970s, when it became law to fly women out of their communities to deliver in hospitals. These days, only pregnancies deemed high-risk require a medevac. (An expectant mother in Puvirnituq with high blood pressure would be flown eight hours to Montreal.)
Leah Unaluk was born in Moose Factory, Ontario. Her mother spent about a month there. It was standard for women to be flown out around the 37-week mark. “I think she was all alone, not knowing people there. She left her friends and family to deliver in a very different environment,” Unaluk says.
Women in small communities in the Yukon, Northwest Territories and Nunavut have much the same experience. The majority of pregnant women leave for regional centres or southern cities weeks before their due dates.
Midwifery hasn’t really caught on in the territories. The Yukon lacks regulations to allow midwives to practice. In the NWT, Hay River and Fort Smith each have successful programs, but plans to expand to other regions have been held up indefinitely. Rankin Inlet has the longest running midwifery program in Nunavut, followed by Cambridge Bay, which hosted Nunavut Arctic College’s Inuit midwifery training program. (It graduated its first two Inuit midwives in 2014.) But after years of being told the safest option was for babies to be delivered in southern hospitals, many women do just that, possibly on the advice of mothers, grandmothers and other relatives. In the decade that followed the opening of the birthing centre in Rankin Inlet in 1993, only half of 1,587 Kivalliq babies were born there. The rest were delivered in Winnipeg or elsewhere. Midwives are required to attend 50 births over a five-year period to maintain their licence, which is often cited as a concern when developing programs in regions with low populations.
But in 1986, Puvirnituq (population 1,700) developed a maternity department and education program in which southern midwives trained local women to carry on the practice. Centres in Inukjuak, Salluit and Kuujjuaq, Québec followed in 1998, 2004 and 2009, respectively.
It’s worked. Unaluk has had all five of her children in Puvirnituq. Tom was the 3,000th baby born at the Puvirnituq Maternity Centre, delivered by women who spoke her language and who lived just a few streets down.
–Elaine Anselmi
Who you gonna call?
A nerve centre for the Northwest Territories
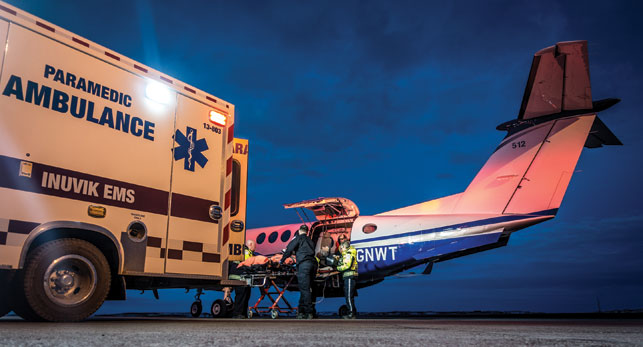
It’s 8:30 a.m. and two calls have already come in for medevacs. The two-person Med-Response team—nurse Karen Brown and dispatcher Kanina Clorey—are seated at computer banks, four monitors wide. They introduce themselves and we chat until a phone rings. In Pavlovian response, they swivel in unison to answer.
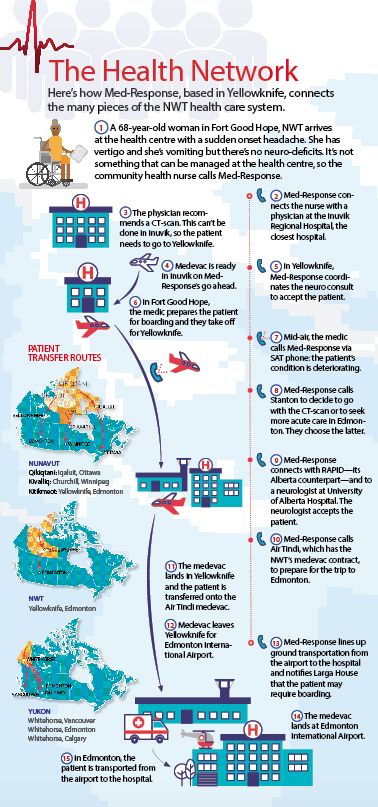
Since 2014, Med-Response has been the nerve centre for the Northwest Territories’ health system. The majority of NWT communities aren’t accessible by all-weather road and even fewer communities have physicians or the facilities required to respond to medical emergencies. That means air ambulances link patients with medical care at regional health centres, the Inuvik Regional Hospital, the larger Stanton Territorial Hospital in Yellowknife or, in the most serious cases, hospitals in Edmonton. Med-Response connects the many moving parts.The call is an update from Air Tindi, which has the medevac contract for the NWT.
Some calls are more complex. Supervisor Susan Rintoul remembers a paediatric case that pulled 13 voices onto a conference call. There were specialists in Yellowknife and Edmonton, a community health nurse and physician in Nunavut, a transport medic, a medical director and an anaesthetist. Some days are more chaotic than others, too. Last December, 14 medevacs stacked up in one day.
Two flatscreen TVs sit above the computer banks. One shows a map of the territory and Alberta where the two active cases are tracked. The other screen displays current weather conditions, which Clorey regularly checks for take-offs and landings.
The phone rings. They swivel. An incoming patient doesn’t speak English, Clorey is informed. She makes a note and then confirms with the health care worker on the line that the patient will have ID before boarding the plane. (Med-Response does not communicate directly with the public.)
A piece of paper taped to the wall reminds staff about weight restrictions, photo ID requirements, and to check if the patient will have an escort. (They also create escort and passenger billing information and coordinate with the medical travel office.) Weight has to be factored in for flights, as do any patient preconditions. And for good reason—like a person with a chest tube has to be flown at a lower altitude. And if a patient from outside the territory, say, has no insurance to cover a medevac flight, they may choose to opt out of the bill, which can run into the five-figure range. The territories are some of the only regions in Canada where medevacs are covered by public health insurance because there really is no other option.
Another call comes in. A baby was born with some minor health complications. The physician just wants to notify paediatrics at Stanton in case its condition changes. Clorey takes down the information and signs off. “Well, congratulations.” – Elaine Anselmi
Help from above
A medevac pilot’s life ain’t easy
All three of Air Tindi’s medevac-dedicated King Air 250s are on the ground in Yellowknife. That’s not uncommon, but it usually means things are about to get busy. “It’s really streaky,” says Jen Reynolds, operational control manager.
There were two medevacs last night. One was called out to Lutselk’e, NWT, a town of 300 on the east arm of Great Slave Lake. Another took a patient from Yellowknife to Edmonton. These twin-engine aircraft, equipped with oxygen and stretcher beds and incubator-compatible, are a lifeline to NWT residents, in 33 communities spread across 1.346 million square kilometres—an area more than twice the size of France.
Flying these planes isn’t for everyone, though. On-call pilots only have 20 minutes to get to the hangar when a call comes in. (They should be “wheels up” within 45 minutes.) That can mean running out of the gym without a shower or abandoning a half-full shopping cart in a grocery store aisle. (An important job requirement is keeping your cell phone charged.)
Their maximum duty time is 14 hours, with a Transport Canada-mandated 10 hours of rest, which can make the job of flight coordinators tricky at times. Brad Unrau, assistant chief pilot of the King Air group, says plans can quickly change. Recently, he got called to Aklavik. Since the hamlet doesn’t have a fuel store for them, they had to make a stop in Norman Wells en route. They brought the patient from Aklavik to Inuvik and as they were set to return to Yellowknife, a call came in for a pick-up in Tuktoyaktuk—another community without fuel.
Roughly half the flights are patient transports from Stanton in Yellowknife to Edmonton. (This could be anything from a woman experiencing pregnancy complications to an emergency visit to a cardiologist.) The rest are medevacs from communities to the hospitals in Yellowknife or Inuvik.
These flights can pose some challenges. Two airstrips (Nahanni Butte and Jean Marie River) aren’t long enough for the King Air 250, so a Twin Otter fitted with medical emergency gear is dispatched. And Fort Providence doesn’t have anyone to report the weather, so pilots will call community nurses for an observation. “Is it snowing outside? Can you see the stars?” Unrau will ask them. “They’re used to it,” he adds. There’s no ambulance in Wrigley, so patients are shuttled to the airport in the back of a pick-up truck. In winter, that can cause IV lines to freeze up. (Some communities like Colville Lake lack nurses, so calls can also come in that aren’t exactly emergencies.) Reynolds recently met with officials from the territorial infrastructure department, who asked what communities needed to make their jobs safer.
Any complications in such an immense territory can be the difference between life and death. Last February, they responded to a highway accident in the Deh Cho by flying the King Air from Yellowknife to Fort Simpson with paramedics from Advanced Medical Solutions (their medevac partner) on board. From there, the medics took a helicopter—operated by Air Tindi’s sister company Great Slave Helicopters—to the highway accident site and transferred the two critical patients to Fort Providence, where the King Air was waiting to rush them back to Yellowknife.
This coordinated response saved a life. –Herb Mathisen
Wellness fit for a town
A creative thinker in Cambridge Bay
Janet Stafford-Brenton leads me into a room with a long table surrounded by about a dozen leather office chairs. This is where the Cambridge Bay Wellness Centre delivers its daily breakfast program, she says. The breakfast table has taken the place of a hospital bed.
“I don’t need an office.”
We pass the food bank storage, located in an old pharmacy from the building’s former life as a health centre. There’s a thrift shop overflowing with toys and clothes across the hall. Stafford-Brenton’s old office was way too big for her, so she had it converted into a drop-in centre for homeless men to stay warm during the hamlet’s long winters. “I don’t need an office,” she says.
Out of this building, staff run some 60 programs. Every room in the wellness centre has been shaped with intention. The walls have been painted warm colours and rugs were rolled over the linoleum floors to do away with the building’s clinical stigma—as a place you go when you’re sick. Staff and client photos cover the walls next to vibrantly painted char welded together by young local artists from scrap metal at the dump.
“Each community has its own specific needs,” says Stafford-Brenton, wellness director for the last six years. Homelessness and food insecurity are priority areas in Cambridge Bay. But she doesn’t rely exclusively on funding from governments for programs because they might be too rigid to address what the community actually requires. Instead, she gets creative.
For instance, last summer Stafford-Brenton oversaw a 28-day on-the-land addictions treatment program that blends Health Canada clinical programs and cultural healing practices. Previously, a resident struggling with alcohol addiction would have to travel south for a month of counselling sessions in a foreign setting. “Every time they were supposed to fly out, they wouldn’t go,” she says. Now, they get outside the four walls and go fishing during the day and talk about what’s happening in their lives. “I find that more people are open when we’re just doing lifeskills,” she says.
Everyone told her it would take years to make the program happen, but she wasn’t having it. As part of the Indian Residential School Settlement Agreement, survivors got $3,000 in credit to put toward an educational or cultural program of their choosing. A few students put theirs toward a cabin eight kilometres outside of town for the wellness centre and it snowballed into a rent-to-own arrangement. Then, eight local men built tent frames out there and went through addictions treatment themselves. The centre now rents the cabin out to government agencies for team-building exercises. This helps pay for supplies and salaries. And wellness staff go out for fun fishing retreats. Their catch goes to the food bank. Every part works to benefit the whole.
The centre’s annual budget has grown to $3.2 million and staffing has climbed from eight to 47 employees in the last five years. Stafford-Brenton is gearing up for proposal- writing season; she does all the reporting. She counsels clients too. As we chat, staff pop their heads in to ask questions. She knows where to find every set of keys, which rooms need cleaning, who in town could really use a visit right now. “You have to know everyone’s role completely,” she says, and how that fits within the larger community.
And that’s what she tells people from hamlets in the Yukon and NWT when they call her about developing their own on-the-land treatment centres. She can share what she did, but she can’t do it for them. That’s got to come from the community. –Herb Mathisen










